The Concussion Spectrum: Who is on the Team?
Published on: April 11, 2019
If you have attended one of our Concussion workshops you know that we embrace the so-called “Concussion Spectrum”. The Concussion Spectrum essentially describes the responsibilities of a concussion management plan that range from prevention strategies to post-concussion psychosocial manifestations to a return to work, school, activity, and life!
It is 2019, and an acceptable buzz term as well as a required standard in many professions is now “Inter-Professional”. To be honest, some professions are truly more inter-professional than others. Some are new in the game, teaching students in a classroom made up of different disciplines and calling it inter-professional. Others in college and university settings prepare inter-professional events based upon the degree disciplines being offered in the respective institution of higher learning. The same can be said about a clinical or hospital-based setting, where inter-professional care is based upon what providers make up the health care team.
In teaching various aspects of concussion management planning to a host of professionals made up of different disciplines all over the world for some two decades now, I have come to learn that many people have a role in management of patient’s who sustain a concussion. In truth, no one person or discipline possesses the skills required to manage all aspects of a concussion. Concussion does not discriminate in age, gender, race, occupation, activity, or any other life variable.
What is your role? Are you involved with equipment fitting, cervical strengthening, or vision training in an effort to minimize the number and severity of concussions? Are you on a field (sports field, highway) assessing acute concussions seconds to minutes after they occur? Are you in an emergency room or clinic office using imaging techniques or office-based assessment guidelines to make an accurate and timely diagnosis? Are you performing post-concussive rehabilitation interventions addressing one of the 6 recognized trajectories (vestibular, cognitive/fatigue, post-traumatic migraine, ocular, cervical, anxiety/mood) of a concussion?
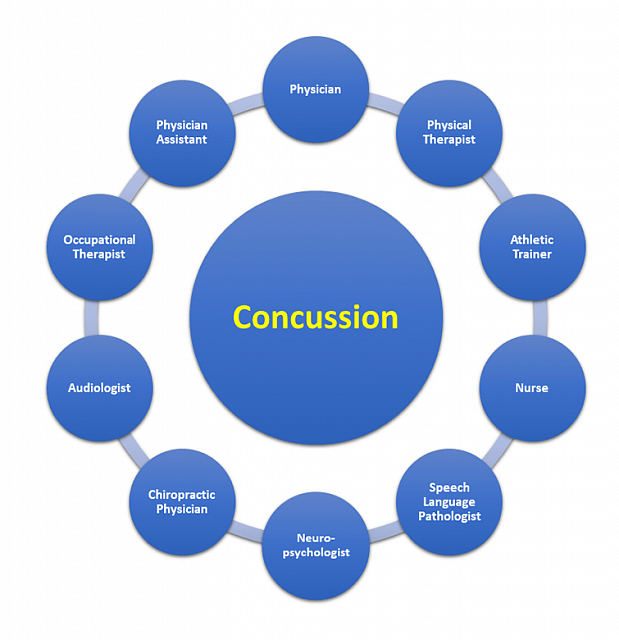

In the end, it is not about us. Rather, it is about the patient, and how “we” can best provide optimal care. “We” being the concussion team. That is why we at AIB embrace collaborative inter-professional care for the patient with a concussion. In building our team, we include the necessary disciplines based upon the patient’s needs. When you build your team, be sure to look beyond the walls of your own environment. If there is ever a time, or a medical condition, that screams for health care professions to work together, it is now and it is concussion!