Review of Diagnostic Tests
 Audiologic Testing
Audiologic Testing
Audiology tests can provide information about hearing, middle ear function, cochlear hair cell function and several neural aspects of the hearing-balance system. Although there are many ear related conditions, which cause hearing loss along with vertigo, there are many that do not. So, the presence of an accompanying hearing loss with the vertigo symptoms may help differentiate certain ear disease-disorders from one another. For example, Menieres disease and labyrinthitis typically has both hearing loss and vertigo, whereas vestibular neuronitis and BPPV only have the symptom of vertigo. Audiology testing often includes: Pure tone (air and bone) and word discrimination tests as well as Immittance Audiometry which evaluates middle and inner ear and some neurological pathways. Otoacoustic Emissions is a relatively new test that looks at the outer hair cell function within the inner ear (cochlea). Brainstem Auditory Evoked Response (BAER) tests the neural conductivity of the hearing and balance nerve (CN VIII).
Gans Sensory Organization Performance Test (SOP)
A combination of the Romberg, clinical test of sensory integration of balance (CTSIB) and Fukuda Stepping Tests provide qualitative information on whether an equilibrium dysfunction exists, whether it is CNS or peripheral and also serves as an indicator of impact on balance function. Whether the is patient surface or visually dependent gives insight into the status of the vestibular system. Recovery of function post treatment may also be documented.
Computerized Dynamic Visual Acuity Test (CDVAT)
This tests for a change in vision with controlled head movement. Oscillopsia is a breakdown in gaze stabilization during active head movement caused by peripheral or central vestibular disorders. The abnormal vestibulo-ocular reflex (VOR) function of as little as 3 degrees can change vision from 20/20 to 20/200 simple head movements. The vision test is conducted while the patient produces horizontal and then vertical head movement of 2.5 cycles per second. This is in the low-mid range of normal active head movement. The test indicates the function problem caused by the vestibular dysfunction and can be used as a baseline to latter compare improvement post Vestibular Rehabilitation Therapy (VRT) to document the treatment efficacy.
Vestibular Autorotation Testing
VOR function gain and phase is quantitatively analyzed using this active rotation test for both horizontal and vertical head movements over a frequency range of approximately 2-8 cycles per second. This indicates the direction of head movement, which is most dysfunctional as well as the frequency (speed) of head movement. The patient is required only to look straight ahead while moving their head to an auditory cuing signal. This test as those mentioned above provides diagnostic as well as outcome measurements. This test can be obtained through passive tests like the Rotary Chair, in which the patient simply sits while being harmonically accelerated or active tests, in which the person volitionally moves their head to an auditory cue.
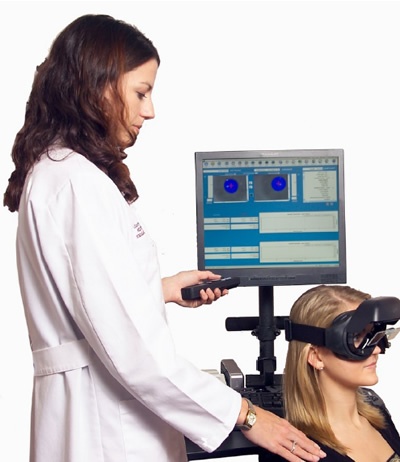
Videonystagmography (VNG)
The most enduring and commonly used test of vestibular function is the VNG. The latest technology utilizes infrared video cameras recording the movement of each eye. Prior to this technology, the test was called ENG, as it was a recording of the corneoretinal potential. The test is comprised of subsets, which include the following:
- Dix-Hallpike – tests for BPPV-PC
- Ocular motor tests – saccadic, pendular and optokinetic pursuit are tests, which provide diagnostic information about the central vestibular and neuropthamologic systems connections within the brain.
- Gaze testing – tests for the presence of spontaneous nystagmus.
- High frequency headshake test – dynamically provokes nystagmus in some cases if the patient has an uncompensated or non-stabilized unilateral vestibular dysfunction.
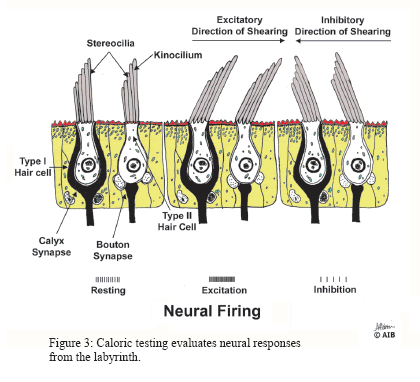 Positional testing – documents the presence of static positional nystagmus. Findings are used for differential diagnosis of HC-BPPV and other peripheral type causes vs. CNS lesions.
Positional testing – documents the presence of static positional nystagmus. Findings are used for differential diagnosis of HC-BPPV and other peripheral type causes vs. CNS lesions.- Caloric tests – Thermal convection of inner ear fluids are created by irrigating each ear with warm and cool air, which is above and below body temperature. The test may also be performed with water. The reactivity or responsiveness of each of the respective ears horizontal semicircular canals is calculated through a measurement of the patients induced nystagmus. A difference of 25% or more in the total nystagmus of the two ears indicates a caloric weakness a finding usually attributed to a peripheral or central dysfunction. In some disorders, both ears responses are depressed.
- Vestibular-Evoked Myogenic Potentials (VEMPs)
Vestibular-evoked myogenic potential testing (VEMPs) is based on the reflex, which occurs between the otolith system (specifically the saccule), and the sternocleidomastoid muscle (SCM). The vestibulo-collic reflex (VCR) has been well studied in animals and humans. The benefit of VEMPs is there is no other vestibular function test, which provides information regarding the saccule or its innervation by the inferior branch of the vestibular nerve. As the VCR is a classic reflex arc with a sensory, CNS, and motor output component, it has been used to provide information regarding both the integrity of the saccule and inferior vestibular nerve, as well as the reflex arc through the brainstem. This has provided information on both otologic and neurologic conditions. In the literature, you will see VEMPs reported in studies with patients ranging from otologic conditions such as Menieres, superior canal dehiscence syndrome to neurological disorders such as multiple sclerosis (MS).